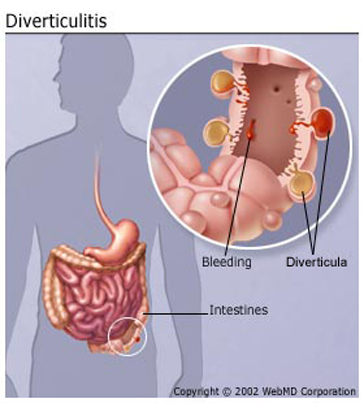
Diverticular diseases stem from conditions related to diverticulosis. This is when pockets, “diverticula,” form in the walls of your digestive tract. Most often they appear in the colon, the lower part of the large intestine. Pressure in the intestine causes the inner layer to push through weak spots in the outer lining. This makes the areas bulge out, and creates little pouches.
Diverticular disease grows more common with age. About 10% of people over age 40 will get diverticulosis, and 50% will get it after age 60. It affects nearly everyone over 80.
There are two main types of diverticular disease -- diverticulitis and diverticular bleeding.
Diverticulitis
This can happen when waste -- bacteria or small pieces of stool from bowel movements -- gets trapped in the pockets. A sac also can tear, or you can lose healthy bacteria in your colon while harmful bacteria increase.
All these factors can cause painful swelling, infection, or irritation in the area.
Some of the main complications that can occur with diverticulitis include:
- Abscess (the pocket fills with pus)
- Rectal bleeding (blood passes through your anus).
- Stricture (your colon narrows so stool can’t pass easily).
- Fistula (a channel that forms to another organ, or the skin -- for example, from the colon to the bladder).
- Most of these conditions require surgery.
Diverticular Bleeding
Blood vessels carry blood from the muscle layer of the lining to the inner wall. If one of the vessels leading to the pocket bursts, lots of blood might suddenly show up in your stool.
It may be dark red, or come in bright red clots. It’s not likely you’ll have any pain, but the sudden blood loss can make you feel weak or lightheaded.
The bleeding will probably stop on its own. But you’ll still need to see your doctor as soon as you notice blood. If the bleeding doesn’t stop, you might need:
- An IV
- Blood replacement (transfusion)
- Other medicine
- Surgery
If you take aspirin more than four times a week, you could have more chance of bleeding.